Click to Read Full Article:
Dr. Mehmet Demircioglu
Diamond Hair Clinic, Istanbul, Turkey
Hair Transplant Consultation
WhatsApp: 0546 840 41 75
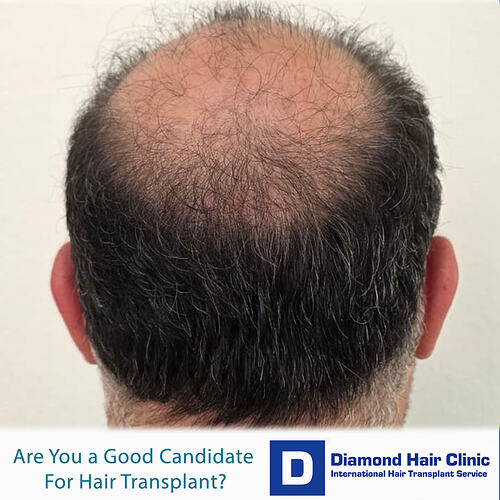
Are You Really a Good Candidate for a Hair Transplant?
One of the most common misunderstandings I see in hair transplantation begins very early, often before a patient has even had a proper consultation with an experienced surgeon.
He starts with the wrong question.
He asks, “How many grafts do I need?”
At first, that may sound like a sensible question.
In fact, it is one of the most common questions in this field. Patients see graft numbers online patient forums and Reddit, compare themselves to other men, look at before and after photos, and naturally begin to think that the whole subject can be reduced to a number.
But in my opinion, that is usually not the right place to begin.
Before talking about graft numbers, coverage, or density, I think a more important question must be answered first:
Are you actually a good candidate for a hair transplant?
That question matters much more than many people realize, because hair transplantation is not simply a matter of moving grafts from one place to another. It is not a mechanical procedure in which the same formula works for everyone. It is a matter of diagnosis, donor management, timing, long-term planning, hair characteristics, expectation management, and understanding what surgery can and cannot honestly achieve.
A person may want surgery very badly. I understand that completely. Hair loss does not affect only the scalp. It affects confidence, self-image, social comfort, and how a man sees himself in the mirror. For some men, it becomes a constant mental burden. So when they finally begin researching hair transplantation, it is very natural that they focus on the visible part of the problem and want a direct answer as quickly as possible.
But wanting surgery and being a good candidate for surgery are not always the same thing.
That is a very important distinction.
In real life, not every patient who wants a transplant is suitable for the same type of plan. Some patients are strong candidates. Some are reasonable candidates, but only with a more conservative design. Some may need medical treatment first before surgery should be considered seriously. And some, in my opinion, should not be having surgery at all, at least not under the plan they currently imagine.
This is exactly why I believe candidacy should be judged much more carefully than many clinics judge it.
If a patient does not have one of the favorable characteristics I mentioned in this article, that does not automatically mean he cannot have a hair transplant. But it may mean the case is more difficult, the margin for error is smaller, the planning must be more cautious, or the expectations need to be adjusted.
And that is precisely why I wrote this article.
Because in hair transplantation, the real first question is often not how many grafts.
The real first question is whether the surgery truly makes sense for you, your donor area, your hair loss pattern, your age, your long-term future hair loss, and what can realistically be achieved naturally without forcing healthy limits.
That is where a proper discussion should begin.
At Diamond Hair Clinic, this is how I believe hair transplant candidacy should be evaluated from the beginning.
At a Glance
A strong candidate usually has:
a stable diagnosis, a reasonably strong donor area, manageable future progression, and realistic expectations.
A weaker candidate often has:
active or unstable hair loss, poor donor quality, unrealistic goals, or a plan that does not make long-term sense.
Why Do I Think the Candidate Question Comes First?
Because the donor area is limited. That single fact shapes almost everything in hair transplantation.
This is the reality behind every hair transplant, no matter how attractively the procedure may be presented online. We are not creating new hair. We are not increasing the total number of grafts a patient has. We are working with a finite supply, and the entire logic of hair transplantation depends on how that limited supply is understood, respected, and used.
The back and sides of the scalp give us the donor reserve. That reserve is valuable, but it is not endless. If it is used intelligently, a patient can achieve a very meaningful and natural improvement. If it is used carelessly, the patient may gain some short-term coverage but lose something far more important in return: donor strength, future flexibility, and the ability to make better decisions later.
That is why I do not like simplistic thinking in this field.
I never like to look only at the bald area and say, “Yes, we can put grafts there.”
That is too superficial.
Because the real question is not only whether grafts can be placed in the thinning area. The real question is whether doing so makes sense when the entire scalp is considered as one long-term picture.
Before I consider how many grafts may be needed, I want to understand what lies behind that bald area. I want to know how strong the donor really is, whether the donor looks stable, whether there are signs of miniaturization, how aggressive the hair loss pattern seems to be (Norwood 1-7), how old the patient is, how likely the hair loss is to progress further, and what the patient is actually hoping to achieve.
These details matter because a hair transplant is not just a technical act. It is a decision about how to spend a limited biological resource, donor grafts.
And that resource must be spent with judgment.
A patient may have a bald frontal area and still be a weak candidate if the donor is poor, the loss is progressing quickly, or the expectations are unrealistic. Another patient may have a larger bald area and still be a better candidate because the donor is stronger, the pattern is more stable, and the goal is more reasonable. This is why I do not believe candidacy can be judged solely by the bald area.
In my opinion, hair transplant surgery candidacy should always be judged by the balance between the area needing help (graft implantation) and the donor reserve (graft extraction) that will be asked to provide them.
That balance is everything.
Because once grafts are taken from the donor reserve, they are taken. Once the donor is unnecessarily weakened, there is no way to restore the lost donor reserve. And once a patient has been pushed into a plan that used too much donor capacity too early, the problem is not only what was done today, but what will no longer be possible tomorrow.
This is why I believe the candidate question comes before the question of how many grafts.
Not because graft numbers do not matter, but because graft numbers only become meaningful after the larger question has been answered properly.
Does this patient truly have the donor quality, the hair loss pattern stability, the long-term outlook, and the realistic expectations for surgery to make sense?
Is the Diagnosis Even Correct?
Before I talk about graft numbers, density, or coverage, I first want to understand a much more basic question:
What kind of hair loss am I actually looking at?
This is extremely important because, in hair transplantation, a good plan can only begin with an accurate diagnosis. If the diagnosis is wrong, everything built on top of it can be wrong as well, including the decision to operate, the hairline design, the graft distribution on the scalp areas, and the expectations.
Many patients assume that every thinning scalp is simply male pattern baldness. Very often, that is true. In daily practice, most men who come for consultation do have androgenetic alopecia, meaning the typical patterned form of hair loss that affects the temples, frontal area, mid-scalp, and sometimes the crown (vertex).
But not always.
And this is where caution matters.
Not every patient with visible thinning should go directly toward surgery. Sometimes the thinning is more diffuse, more unstable, or less predictable than it first appears. Sometimes the scalp may show signs of inflammation or another underlying condition that changes the entire meaning of the case. Sometimes the donor area itself may already be showing weakness, miniaturization, or instability. In some patients, this may even suggest DUPA (Diffuse Unpatterned Alopecia).
And sometimes the patient’s photos may create a much simpler impression than the real scalp examination does.
This is exactly why I do not like to make fast, superficial judgments.
A hair transplant makes the most sense when the patient has a type of hair loss that is compatible with surgery, when the pattern is stable enough to plan responsibly, and when the donor area is strong enough to support the work. But if the real problem has not been properly understood, surgery can become a very poor answer to the wrong question.
That is why a proper consultation matters so much.
I do not want to look only at a few photographs and say yes or no too quickly. I want to understand the pattern, distribution, progression rate, donor quality, scalp condition, and the likely future direction of the case. I want to know whether I am looking at a straightforward surgical case or one that requires greater caution, additional medical management, or more time.
Because a patient is not a good candidate simply because he is losing hair.
He is a good candidate only if the type of hair loss, the stability of the situation, and the quality of the donor area all support surgery in a sensible way.
In my opinion, this is one of the biggest differences between a serious medical assessment by a surgeon and a sales-driven assessment by call center staff.
A sales-driven approach sees hair loss and quickly moves to graft numbers.
A proper medical approach first asks, what exactly is happening on this scalp, and does surgery truly make sense here?
That is the right order.
Because when the diagnosis is clear, the rest of the plan becomes more intelligent. And when the diagnosis is unclear, rushing toward surgery can create problems that were avoidable from the beginning.
Why Do Some Patients Look Like Candidates Online but Not in Reality?
Because the internet is a very incomplete way to judge hair.
Online photos can be useful. They help create a first impression. They may show the general pattern of loss, the frontal recession, the crown involvement, or the broad appearance of the donor area. For an initial conversation, that can be helpful.
But they never show the whole reality.
A patient may appear to be a strong candidate in a few photos, but once properly examined, the case may look very different. The donor area may be weaker than it appeared. The side zones may be thinning more than expected. The scalp may show subtle inflammation or signs that the situation is less straightforward than the photos suggest. The level of miniaturization may be more advanced. And the apparent density may be helped by hair length, styling, lighting, fibers, or simply the angle from which the photos were taken.
All of these things can change how a case looks.
This is why I am always cautious about judging candidacy too quickly from online images alone.
A photograph can make a patient look simpler than he really is.
And sometimes it can make a weak situation look deceptively strong.
For example, a donor area may appear dense in a few routine photos, but on close examination, the density may be lower than expected, the caliber may be finer, or the donor may show early signs of instability. A thinning frontal area may appear to be a straightforward case for surgery, but in reality, it may be part of a more diffuse, active process that requires a more careful approach. Even something as basic as bright light, longer hair, or careful combing can make a patient seem like a better candidate than he actually is.
This is also one of the reasons I often tell patients not to judge hair transplant results too quickly based on random online images.
The same problem exists on the result side as well.
A photo may make a result look extremely dense, but the image may reflect ideal lighting, dry hair, styling tricks, or angles that hide what the scalp looks like from other directions. In the same way, a patient may appear to be a strong candidate in a few consultation photos, but that impression may not hold up under closer examination.
So yes, photos are useful.
But they can also create false confidence.
They can make a patient believe the case is more straightforward than it really is. They can make the donor look stronger than it really is. And they can make the likely result seem easier to achieve than it really is.
That is why, in my opinion, candidacy should never be judged too casually from internet images alone.
A patient who looks simple online may turn out to be a much more delicate case in reality.
And that is exactly why proper examination, careful assessment, and real medical judgment matter so much in hair transplantation.
Why Can Two Patients With the Same Norwood Level Be Completely Different Candidates?
This is a very important point, because many patients look at the Norwood scale and assume it tells the whole story.
It does not.
The Norwood scale is useful, of course. It helps describe the pattern and extent of visible hair loss in a general way. It gives us a common language. When I say a patient is Norwood 3, 4, or 5, that communicates something meaningful.
But it does not tell me everything I need to know to judge whether that patient is actually a good candidate for surgery.
And that distinction matters a lot.
Two patients may both be Norwood 4, but one may be a very reasonable candidate, and the other may be a much more difficult case. On paper, they may appear similar. In reality, they may be completely different from a surgical standpoint.
Why?
The Norwood scale only tells me how hair loss looks in a broad visual sense. It does not fully tell me the donor density, the hair caliber, the curl, the texture, the contrast between the hair and the scalp, the degree of miniaturization, the strength of the side zones, whether there is retrograde thinning, how aggressive the future progression may be, or whether the patient’s expectations are realistic.
And all of those things matter.
One Norwood 4 patient may have thick, wavy hair, low scalp-hair contrast, strong donor density, and a stable pattern that has progressed slowly over the years. Another Norwood 4 patient may have fine hair, high contrast between hair and skin, donor miniaturization, retrograde hair loss, weak side support, and aggressive, ongoing thinning.
These are not the same cases.
Not even close.
The first patient may achieve a very satisfying visual improvement with relatively efficient use of grafts because his hair characteristics work in his favor. The second patient may need a much more cautious discussion because, even with surgery, the same number of grafts may produce a weaker visual effect, the donor may be less reliable, and the long-term outlook may be more uncertain.
This is why I never like simplistic comparisons between patients.
A patient may say, “I saw somebody online who was Norwood 4 like me, and he had 3,500 grafts, so I should need the same.”
But that is not how real hair transplantation works.
Because two men can share the same Norwood level and still have very different biology, donor strength, and surgical outcomes.
This is also why I do not like judging candidacy only from the front-facing appearance of baldness. The visible recession is only one part of the case. What matters just as much is the quality of the remaining hair, the donor’s character, and how the case is likely to evolve over time.
In my opinion, the Norwood scale is a useful starting point, but only one.
It helps describe the map, but it does not tell me how strong the roads are, how much fuel is available, or whether the journey is actually safe.
That is why I never judge candidacy by the Norwood level alone.
I judge it by the full picture.
And the full picture is always more important than the label.
Why Do I Look So Carefully at the Donor Area?
Because the donor area is the budget.
That is still the simplest and most honest way to explain it.
In hair transplantation, everything depends on what the donor area can safely give. The back and sides of the scalp are not just another part of the head. They are the reserve of “DHT-Resistant Hair Grafts” that make the entire procedure possible. So before I think seriously about what can be built in the front, I first want to understand what stands behind it.
If the donor area is strong, dense, and stable, then we have more freedom. We can usually plan with greater confidence, use the grafts more intelligently, and still preserve room for the future. But if the donor is weak, sparse, miniaturized, or otherwise questionable, then every decision becomes more delicate because the margin for error is much smaller.
Many patients naturally focus only on the front. That is understandable, because that is the part they see in the mirror every day. They see the recession, the thinning, the change in framing around the face. But in hair transplantation, the front is only half of the story.
The other half is this: What was spent behind to create what you see in front?
That question matters enormously.
A result may look attractive in a photo taken from the right angle, but if too much donor was consumed to create it, then the long-term logic of that result may be poor. The patient may be left with a thinner donor area, reduced future flexibility, and a much weaker position if the native hair continues to thin later.
This is exactly why I do not like aggressive and careless approaches.
Some clinics behave as if the donor area is an endless field that can be harvested freely. It is not. The donor is a limited biological resource. Once grafts are removed, they are removed. Once the donor is weakened unnecessarily, that loss is not easy to undo. And if the donor is handled poorly during the first surgery, the patient may continue paying for that mistake years later.
This is why, in my opinion, donor management is not just a technical detail. It is one of the central signs of whether a clinic is thinking responsibly.
When I assess candidacy, one of the first questions I ask myself is this:
Does the donor truly support the plan, or is the patient asking the donor to do more than it can safely do?
That is a very important distinction.
Because sometimes the visible bald area creates pressure for a large plan, but the donor simply does not justify that plan. In those cases, the honest answer is not to force the donor to comply with the patient’s wishes. The honest answer is to respect the donor’s limit and build the strategy around reality.
I also look carefully at the donor because not all donor areas are equal. Two patients may appear similar from the front, but once I examine the donor more closely, the difference may become very clear. One may have stronger density, better caliber, and better long-term reliability. The other may already show weakness, reduced density, or signs that the safe reserve is narrower than it first seemed.
That is why I never judge a case only by how bald the recipient area looks.
In my opinion, a hair transplant should always be planned as a balance between what is needed and what can be safely supplied. And that balance can only be judged properly when the donor area is examined with great care.
Because in the end, the success of a hair transplant is not determined only by what is implanted.
It is also determined by what was preserved.
What If the Donor Area Itself Shows Weakness?
This is a very important red flag.
When I evaluate a patient, I do not look at the donor area only in terms of how full it appears from a distance. I also want to understand how stable it truly is. Because a donor area can look acceptable at first glance and still contain a deeper problem underneath.
If the donor area itself shows miniaturization, the case changes immediately.
Why?
Because then the donor may not be as secure as it first appears. And once that becomes part of the picture, the question is no longer only how much hair can I extract? The question also becomes how reliable is that donor hair over the long term?
That distinction matters a great deal.
Hair transplantation relies on the premise that donor hair is relatively more resistant and dependable. But if the donor itself is beginning to show weakness, then the long-term value of the surgery becomes more questionable. In practical terms, I may be taking hairs that look usable today, but that may themselves already be on the path toward thinning later.
And if that happens, the patient may go through surgery, use part of his donor reserve, and still not receive the stable long-term benefit he expected.
That is why this issue matters so much.
Because a weak donor is not just a matter of quantity.
It is also a quality problem.
In other words, the concern is not only whether I can extract a certain number of grafts. The concern is whether those grafts are truly worth extracting in the first place.
This is why I like to examine the donor area carefully and not judge it casually. It is not enough for the donor to look simply “full enough” in ordinary photographs. Photos can be misleading. Hair length can hide weakness. Lighting can flatter the area. Styling can make density look stronger than it really is.
I want to know how strong the donor really is.
I want to understand whether the density is genuinely supportive, whether the caliber is strong enough, whether the pattern looks stable, and whether there are signs that the so-called donor zone is not as safe as it may appear at first glance.
Because once I begin extracting from a weak or unstable donor, I am not just risking a thinner donor appearance later. I may also be building the surgery on a less reliable foundation from the beginning.
And in my opinion, that is a dangerous way to plan a case.
This is one of the biggest differences between a superficial assessment and a serious one.
A superficial assessment may say, “The back looks fine, so let’s use it.”
A serious assessment asks, “Does this donor actually have the long-term strength to support surgery responsibly?”
That is the better question.
Because if the donor area itself shows weakness, then I have to become much more cautious. Sometimes that means the plan needs to be made more conservative. Sometimes it means the patient needs further observation or medical treatment first. And sometimes it means the surgery should not be pushed at all.
So yes, donor weakness is a very important red flag.
Not because it automatically makes surgery impossible.
But because it changes the case from something straightforward into something that demands much more restraint, much more judgment, and much more honesty about what surgery can realistically offer.
Why Does Retrograde Hair Loss Matter So Much?
Because it affects both the supply and the design, and that makes it much more important than many patients realize.
A lot of men think about hair loss only in terms of what is happening on the scalp. They focus on the temples, the frontal recession, the mid-scalp, or the crown. That is understandable, because those are the areas that usually attract the most attention.
But in some patients, the story is broader than that.
When hair loss begins extending lower on the sides, receding toward the ears, or moving upward from the nape, the case changes in a very important way. This is what makes retrograde hair loss such a significant finding.
The first reason is practical.
If hair loss is progressing into areas that would normally help define or support the donor zone, the safe donor reserve may become smaller. That means the surgeon may have fewer truly reliable grafts available for extraction. In other words, the supply side of the equation becomes weaker.
And that alone is already important.
But that is only one part of the problem.
The second part is aesthetic, and in my opinion, this is where many patients underestimate the issue.
If the side support is weakening and the surgeon tries to rebuild only the front, the result may start to look disconnected. A frontal hairline does not exist in isolation. It is not just a line drawn across the forehead. It has to connect naturally with the rest of the scalp, the temporal areas, the side profile, and the overall frame of the face.
If that support is missing, the result can begin to look artificial, even if many grafts were used.
A patient may technically have a reconstructed front, but if the lateral areas have receded too far and the overall frame is broken, the transplant can start to look incomplete or unnatural. In some cases, it may create a strange visual impression that the front has been rebuilt, while the rest of the scalp no longer supports it properly.
That is exactly why I do not assess hair loss only from the front-facing angle.
The side profile matters too.
The transitions matter too.
The overall frame matters too.
This is one of the reasons I believe a hair transplant should never be judged solely by whether hair can be implanted in the frontal zone. The real question is whether the result will look coherent as a whole.
And coherence depends on more than a hairline.
It depends on how the frontal work relates to the temples, the sides, the parietal transition, and the visual support that surrounds the face.
Retrograde hair loss also matters because it can subtly complicate planning. Sometimes the patient focuses only on the front and does not realize that the side zones are gradually weakening. But if those areas continue changing, then a plan that looked acceptable at one stage may look much less balanced later.
That is why I take this finding seriously.
Because when retrograde thinning is present, the surgeon has to think more carefully about how much donor tissue truly exists, how stable it is, and whether the intended design will still look natural if the side support continues to weaken over time.
In other words, retrograde hair loss is not just a side detail.
It changes the whole case.
It changes how much of the donor reserve can be safely extracted.
It changes how the frontal work should be judged.
And it changes how honestly the long-term picture must be discussed.
So yes, retrograde hair loss matters a great deal.
Not because it automatically makes surgery impossible.
But because it makes the case more complex, it narrows the margin for error and reminds us that a natural result is not built only from the front. It is built from the entire frame.
Click to Read Full Article:
Dr. Mehmet Demircioglu
Diamond Hair Clinic, Istanbul, Turkey
Hair Transplant Consultation
WhatsApp: 0546 840 41 75
#hairtransplant #fuehairtransplant #hairtransplantturkey #hairtransplantistanbul #hairrestoration #diamondhairclinic #drmehmetdemircioglu